- About Us
- KIDNEY DISEASE
- Public Education
- Treatment
- Patient Welfare
- Training
- Events
- Support Us
- Resources



The main job of your kidneys is to remove toxins and excess water from your blood.
Kidneys also help to control your blood pressure, to produce red blood cells and to keep your bones healthy. Each roughly the size of your fist, kidneys are located deep in the abdomen, beneath the rib cage.
Your kidneys control blood stream levels of many minerals and molecules including sodium and potassium, and help to control blood acidity. Every day your kidneys carefully control the salt and water in your body so that your blood pressure remains the same.
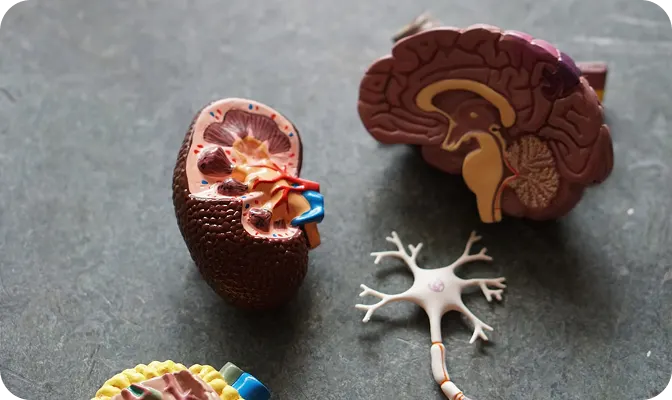
The majority of people are born with two kidneys, each made out of a million tiny units, known as nephrons. When nephrons are damaged, they stop functioning, placing added strain on the remaining healthy nephrons to sustain normal kidney function. However, if the damage continues, the remaining healthy nephrons become insufficient to maintain kidney function.
This progressive loss in kidney function over a span of months or years is called Chronic kidney disease (CKD). CKD is extremely common, with 1 in 10 of the adult population having some form of kidney damage, and every year millions die prematurely of complications related to CKD.
This helps you maintain a healthy weight, lower blood pressure, and reduce the risk of Chronic Kidney Disease.
With active habits such as walking, jogging, or cycling, you can improve blood circulation, strengthen your heart, and support healthy kidney function.
1. Walking 10,000 steps a day can burn up to 500 calories and help regulate blood pressure.
2. Just 30 minutes of moderate exercise, 5 times a week, can reduce the risk of chronic diseases by up to 30 percent.
Activate your body today for a healthier heart, mind, and kidneys.


This can help you maintain a healthy weight, lower blood pressure, and prevent diabetes, heart disease, and other conditions related to Chronic Kidney Disease.
Reduce salt intake. The recommended daily sodium intake is 5–6 grams of salt, including salt already present in processed foods (roughly one teaspoon).
To reduce salt consumption, limit processed foods and restaurant meals that tend to contain added salt.
About half of individuals living with diabetes do not realize they have the condition. This is why monitoring blood sugar should be part of routine health checkups. It is especially important for those at higher risk.
Around half of people with diabetes develop kidney damage — however, this can be prevented if diabetes is well managed from the start.
Check your kidney health regularly through blood and urine tests.


1. According to the National Health and Morbidity Survey (NHMS) 2023, about 29.2 percent, or almost 1 in 3 adults, have hypertension.
2. Among these individuals, 11.9 percent are unaware of their condition.
Blood pressure should be measured during routine health screenings. High blood pressure can damage the kidneys over time, especially when combined with other risk factors such as diabetes, high cholesterol, and cardiovascular disease. This risk can be reduced with proper blood pressure management.
Normal adult blood pressure is 120/80 mmHg. Hypertension is diagnosed when, on two separate days, the systolic reading is ≥140 mmHg and/or the diastolic reading is ≥90 mmHg (WHO).
If your blood pressure remains high (especially in older adults), consult your doctor to discuss risks, lifestyle changes, and medication if needed.
The ideal amount of fluid varies by individual and depends on activity level, climate, health status, pregnancy, and breastfeeding.
In general, this means 8 glasses or about 2 liters a day for healthy individuals in normal climate conditions.
Fluid intake should be adjusted during hot weather. It may also need modification if you have kidney disease, heart disease, or liver issues. Consult your doctor for guidance tailored to your condition.


Smoking reduces blood flow to the kidneys. When blood flow decreases, the kidneys cannot function normally. Smoking also increases the risk of kidney cancer by about 50 percent.
Do not frequently take over-the-counter painkillers. Common medicines such as non-steroidal anti-inflammatory drugs (NSAIDs) or general pain relievers like ibuprofen can damage the kidneys if taken regularly.
If you have kidney disease or reduced kidney function, even small amounts of these medications can worsen your condition. Always consult your doctor before taking them.


You should check your kidney function if you have one or more of the following risk factors:
Acute Kidney Injury (AKI) is the sudden loss of kidney function that occurs within a few hours or a few days.
This sudden decline in kidney function can be caused by various factors, including reduced blood flow to the kidneys or exposure to toxic substances.
The good news is that the kidneys can almost fully recover with prompt treatment. Early management may involve fluid and mineral replacement, and in some cases, dialysis may be necessary.
To prevent complete kidney failure, awareness of AKI must be strengthened, especially among individuals at higher risk. Early detection and treatment are crucial to improving recovery outcomes.
What causes Acute Kidney Injury (AKI)?
AKI has three main causes:
1. A sudden and severe drop in blood flow to the kidneys.
2. Damage caused by medications, toxins, or infections.
3. Sudden blockage that prevents urine from leaving the kidneys.
Who is at higher risk of AKI?
The risk of AKI is higher among:
These conditions can increase the risk of kidney failure.
What are the symptoms of AKI?
Signs of AKI may include:
Some people may not show any symptoms at all. For critically ill patients, the underlying illness may cause symptoms that make AKI harder to detect.
AKI Cases
Worldwide, AKI is common, especially among hospitalized patients. AKI affects 5 to 20 percent of patients in Intensive Care Units and is becoming increasingly recognized globally.

Most organs in our body are closely connected and depend on each other. This includes the heart and kidneys.
There is a strong relationship between kidney disease and cardiovascular disease (heart and blood vessel disease).
People with Chronic Kidney Disease (CKD) have a significantly higher risk of experiencing stroke or heart attack at a younger age, due to changes in blood circulation caused by kidney disease.
What is Cardiovascular Disease (CVD)?
CVD refers to any condition involving the heart and blood vessels. Any issue that prevents the heart from pumping blood effectively can be classified as cardiovascular disease.
Common types include:
1. Atherosclerosis – buildup of fats and cholesterol in the artery walls
2. Thrombosis – blood clots in veins or arteries
3. Heart attack – reduced blood supply causing heart muscle damage
How are Kidney Disease and Heart Disease Connected?
Heart and kidney diseases are closely linked because most organs in the body depend on each other.
People with CKD have a higher risk of stroke or heart attack at a younger age due to circulatory changes caused by kidney damage.
Shared Risk Factors Between CKD and CVD
What are the symptoms of AKI?
Signs of AKI may include:
Some people may not show any symptoms at all. For critically ill patients, the underlying illness may cause symptoms that make AKI harder to detect.
AKI Cases
Worldwide, AKI is common, especially among hospitalized patients. AKI affects 5 to 20 percent of patients in Intensive Care Units and is becoming increasingly recognized globally.

Diabetes is the leading cause of kidney failure.
In many countries, half of all patients starting dialysis have kidney failure caused by diabetes.
What is Diabetes?
Diabetes is a chronic metabolic disease marked by high blood glucose levels. Over time, it can damage the heart, blood vessels, eyes, kidneys, and nerves.
Many people with diabetes also have high blood pressure, which increases the risk of kidney disease.
High blood pressure and diabetes are considered the main causes of kidney damage.
What is Diabetic Kidney Disease?
Uncontrolled diabetes causes high blood sugar that damages the tiny blood vessels in the kidneys, affecting their filtering function.
This condition is known as Diabetic Nephropathy or diabetic kidney disease.
In many cases, early diabetic kidney disease shows no symptoms. The only way to diagnose it is through urine tests to detect albumin (protein). If albumin is detected, blood tests such as eGFR should be performed.
You should test for diabetic kidney disease yearly if you:
Hypertension is the medical term for high blood pressure. For most people, blood pressure of 140/90 mmHg or higher is considered abnormal.
What is Hypertension?
Hypertension occurs when blood pressure against the artery walls is consistently too high.
Normal blood pressure reading: 120/80 mmHg.
Hypertension is diagnosed when the pressure reaches 140/90 mmHg or higher.
How Are Hypertension and Kidney Disease Connected?
Hypertension is one of the main causes of Chronic Kidney Disease (CKD). High blood pressure damages kidney blood vessels, reducing their ability to function properly.
Damaged kidneys cannot remove waste effectively, causing fluid buildup that further increases blood pressure. This creates a harmful cycle.
About 90 percent of people with CKD stages 3–5 have hypertension.
Symptoms of High Blood Pressure and Kidney Disease
Managing blood pressure with medication and lifestyle changes can help prevent CKD progression.
Can Hypertension and Kidney Disease Be Prevented?
Managing blood pressure with medication and lifestyle changes can help prevent CKD progression.

Excess weight increases the risk of developing conditions such as diabetes, cardiovascular disease, hypertension, and kidney disease.
By 2025, 18 percent of men and 21 percent of women globally are projected to be obese.
In some countries, more than one-third of the adult population is obese.
Obesity in children is also rising globally.
What is Obesity?
According to the World Health Organization (WHO), obesity is excessive fat accumulation that may impair health.
It is commonly measured using the Body Mass Index (BMI):
Common types include:
1. Normal weight: BMI 18.5–25 kg/m²
2. Overweight: BMI 25–29.9 kg/m²
3. Obese: BMI 30 kg/m² and above
How Are Obesity and Kidney Disease Connected?
Obesity increases the risk of diabetes and hypertension, which are major causes of kidney disease.
Obesity directly contributes to Chronic Kidney Disease (CKD) by increasing:
1. Type 2 diabetes risk
2. High blood pressure
3. Heart disease
People with obesity have a 2 to 7 times higher risk of developing End-Stage Kidney Disease (ESKD).
Obesity also increases the risk of Acu
te Kidney Injury (AKI).

Organ donation occurs when someone agrees to donate their organs for transplantation, either while alive or after death with consent from next of kin.
Through initiatives like ColdEve by NKF, communities are educated about organ donation and how it can provide a second chance at life.
Who Can Be an Organ Donor?
There are two types of donors:
1. Living donors
2. Deceased
Living donors are healthy individuals aged 18 and above who voluntarily donate an organ after undergoing full physical and mental assessments.
Deceased donors are individuals who have passed away and previously expressed their wish to donate. Only some can donate, depending on suitability.
Deceased donors must be confirmed to have brain death, usually caused by conditions such as:
What Organs Can Be Donated?
Every donation is a gift of life. Living donors may donate:
Most organ donations, however, come from deceased donors.
A deceased donor can save up to eight lives by donating:
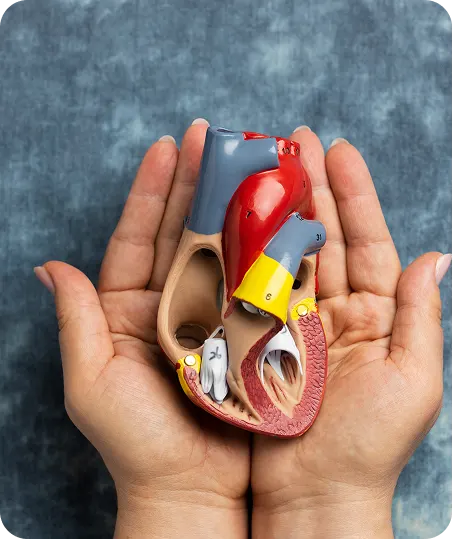
Healthy kidneys filter blood and remove excess fluid through urine. They also produce important chemicals that help keep the body healthy.
Dialysis replaces these functions when the kidneys can no longer work effectively. Dialysis can be done at a dialysis center or at home.
Types of Dialysis
There are two main types:
1. Hemodialysis (HD)
Blood is pumped through a dialysis machine to remove waste and excess fluid. It can be done at:
2. Peritoneal Dialysis (PD)
Uses the lining inside the abdomen instead of a machine to filter waste.
A cleansing fluid is infused into the abdominal cavity to absorb waste, then drained out.
PD is usually done at home. Some patients use a machine called a cycler, especially at night.